Artificial intelligence is quickly becoming part of the Medical Billing conversation — especially when it comes to coding.
Many platforms today promise faster coding, fewer errors, and reduced dependency on human coders. Some even go as far as suggesting that AI can fully automate coding workflows.
But if you’ve worked in real-world billing, you already know:
Coding is not just about matching documentation to codes.
It’s about interpretation, compliance, payer behavior, and context.
So the real question isn’t AI vs human coders.
The real question is:
Where does AI actually help — and where does human expertise still make the difference?
Let’s break that down.
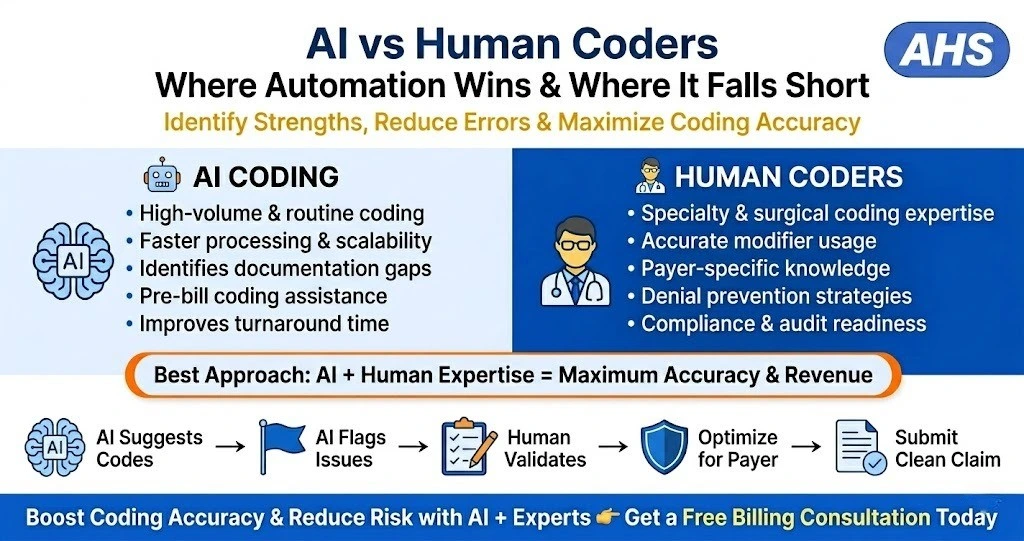
Where AI Wins in Medical Coding
1. High-Volume, Routine Coding
AI performs best in environments that are:
- Structured
- Repetitive
- Well-documented
For example:
- Standard office visits (E/M coding)
- Routine follow-ups
- Preventive care visits
- Simple urgent care encounters
In these cases, AI can:
- Scan documentation quickly
- Suggest appropriate CPT and ICD-10 codes
- Reduce manual effort
- Improve turnaround time
For high-volume practices, this can significantly improve productivity.
2. Speed and Efficiency
AI can process documentation at a scale that humans simply cannot match.
Instead of manually reviewing each note line by line, AI can:
- Extract key clinical elements
- Map them to potential codes
- Highlight missing documentation
- Prepare codes for review
This does not eliminate the need for coders — but it allows them to focus on validation instead of starting from scratch.
3. Identifying Documentation Gaps
One underrated strength of AI is its ability to flag incomplete documentation.
For example:
- Missing laterality
- Incomplete procedure details
- Lack of medical necessity indicators
- Inconsistent diagnosis linkage
Catching these issues before claim submission can help reduce denials and rework.
4. Pre-Bill Coding Assistance
AI works very well as a pre-bill support layer.
Instead of replacing coders, it:
- Suggests codes
- Flags risks
- Highlights inconsistencies
This helps coders move faster and make more informed decisions.
Where Human Coders Still Win
1. Specialty and Surgical Coding
This is where things get real.
In specialties like:
Coding is rarely straightforward.
It involves:
- Multiple procedures
- Bundling and unbundling rules
- Modifier decisions
- Documentation interpretation
- Payer-specific behavior
AI struggles here because:
- Rules are not always consistent
- Payer expectations vary
- Clinical nuance matters
A human coder understands context.
AI mostly understands patterns.
And in specialty billing, context wins.
2. Modifier Usage (The Biggest Gap)
Modifiers are one of the hardest parts of coding — and one of the biggest gaps in AI today.
For example:
- Modifier 25 (separate E/M service)
- Modifier 59 (distinct procedural service)
- Laterality modifiers
- Multiple procedure modifiers
These are not just rule-based decisions.
They require:
- Clinical justification
- Documentation support
- Understanding payer scrutiny
A wrong modifier can lead to:
- Denials
- Audits
- Compliance risks
This is where experienced coders are still far more reliable than automation.
3. Payer-Specific Nuances
AI systems are typically trained on generalized coding logic.
But real-world billing depends heavily on:
- Payer policies
- Local coverage determinations
- Regional variations
- Contract-specific rules
For example:
- What works for Medicare may not work for BCBS
- One payer may bundle codes that another allows separately
- Authorization requirements vary widely
Human coders and billing teams learn these patterns over time.
AI, unless extremely well-trained and customized, often misses these nuances.
4. Denial Prevention Through Experience
A good coder doesn’t just code for submission.
They code for reimbursement.
That means thinking ahead:
- Will this get denied?
- Does this need additional documentation?
- Should we code differently based on payer behavior?
AI can flag risks, but it doesn’t always understand:
- Why a payer denies something repeatedly
- How to adjust coding strategy accordingly
That level of thinking still comes from experience.
5. Compliance and Audit Readiness
Coding is not just about getting paid.
It’s about getting paid correctly and defensibly.
Human coders bring:
- Compliance awareness
- Audit readiness
- Documentation alignment
- Risk judgment
AI can assist with compliance checks, but relying on it entirely can be risky — especially in high-stakes or audited environments.
The Real Answer: It’s Not AI vs Human Coders
The most successful practices are not choosing one over the other.
They are combining both.
AI handles:
- Speed
- Pattern recognition
- Repetitive tasks
- Initial code suggestions
- Documentation scanning
Human coders handle:
- Judgment
- Complexity
- Compliance
- Payer nuance
- Final validation
This combination creates a more efficient and more reliable workflow.
What a Smart Coding Workflow Looks Like Today
A practical, real-world approach looks like this:
Step 1: AI reviews documentation and suggests codes
Step 2: AI flags missing or risky elements
Step 3: Human coder validates, adjusts, and finalizes
Step 4: Billing team reviews payer-specific considerations
Step 5: Claim is submitted with confidence
This is where AI adds value — not by replacing coders, but by supporting them.
What Practices Should Keep in Mind
If you’re considering AI for coding, here are a few practical takeaways:
- Do not treat AI as a replacement for coders
- Use AI to support high-volume workflows
- Be cautious in specialty and surgical coding
- Always validate Modifier Usage
- Ensure strong documentation before relying on automation
- Combine AI insights with real-world billing experience
AI can make your team faster.
But accuracy, compliance, and revenue still depend on people.
Final Thoughts
AI is changing medical coding — but not in the way many headlines suggest.
The biggest gains today are not coming from full automation.
They are coming from AI-assisted workflows.
Where AI wins:
- Speed
- Scale
- Repetition
- Pattern detection
Where humans win:
- Judgment
- Context
- Strategy
- Compliance
The future of medical coding is not about replacing human coders.
It’s about empowering them with better tools.
And the practices that understand that balance will always have the edge.
Looking to Improve Coding Accuracy Without Compromising Compliance?
At Acuity Health Solutions, we combine experienced coding teams with smart workflows to ensure accurate, compliant, and optimized billing outcomes — especially for specialty practices.
If you’re exploring ways to improve coding efficiency without increasing risk, we’d be happy to help.
Get in touch with Acuity Health Solutions to learn more about our medical billing and coding solutions.




