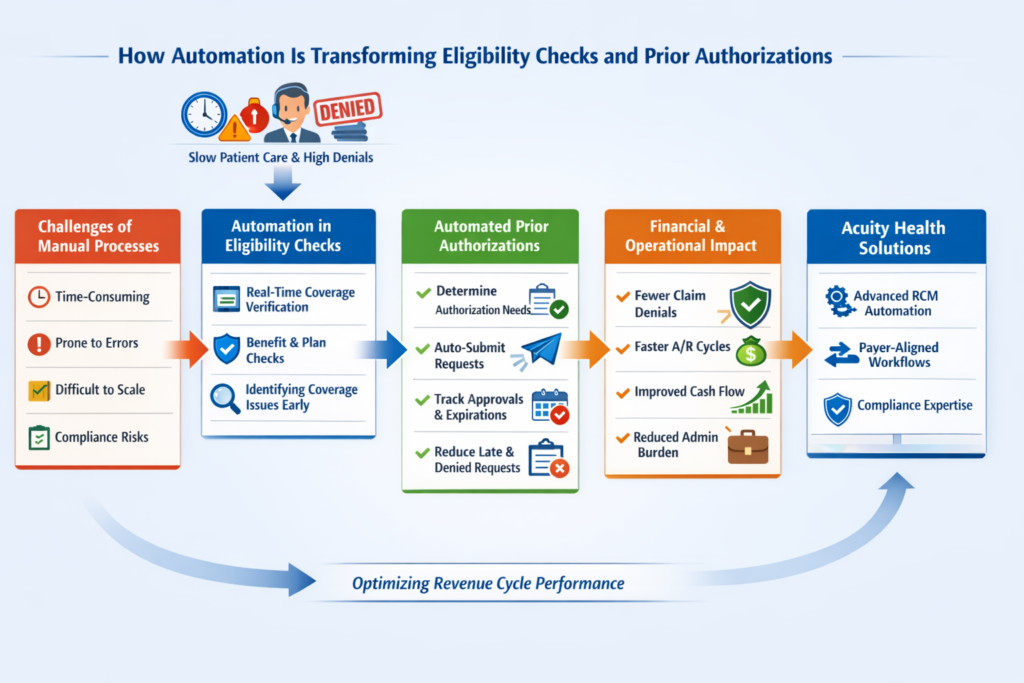
Verifying eligibility and having a prior authorization are two of the most susceptible and time consuming part of the Healthcare Revenue Cycle. When operated manually, they add to the slow delivery of care, unnecessary denials, and burnout among the administration. With more and more challenging payer requirements, automation is also changing this practice of checking eligibility and prior authorizations and making it more accurate, faster, and financially effective.
Why Eligibility and Prior Authorizations Matter in RCM
Documenting eligibility is done to prove that the insurance cover of a patient is in force and to ascertain benefits, copays, deductibles, and limitations on the plan. Prior authorization is a method whereby a payer pre-approves a service before it is delivered. The mistakes during any of the steps may lead to a refusal of claims, failure to pay on time, or failure to pay at all.
The industry statistics have shown that a considerable number of denials are always due to front-end errors, which may include inactive coverage, inappropriate plan selection, or absent approvals. Since these problems arise prior to rendering services, they can be averted in most cases by the appropriate procedures and machinery.
The Limitations of Manual Processes
Paper-based eligibility verification usually has the staff logging in to several payer portals, making phone calls, and deciphering plan benefit characteristics. Prior authorization processes are further disintegrated and usually consist of paperwork, faxing, and payer-directed policies.
These manual processes are:
- Labor-intensive and time-consuming.
- Likely to be misused by humans and have different interpretations.
- Hard to scale between high-volume practices.
- Increasing audit and compliance risk, as it is not well-documented.
The alteration in payer policies has increased the difficulty of maintaining the training of the staff and updating workflows.
Automation to Enhance Eligibility Checks
The automated eligibility systems are directly connected with the practice management systems and payer databases in order to check coverage in real time. They can automatically check the status of the plan, level of benefits, and limitations to cover before the patient is attended to.
How Automation Improves Eligibility Verification
The automated eligibility systems are directly connected with the practice management systems and payer databases in order to check coverage in real time. They can automatically check the status of the plan, level of benefits, and limitations to cover before the patient is attended to.
The primary advantages of automated checks of eligibility are:
- Quicker checking at check-in or scheduling.
- Fewer registration and billing mistakes.
- Definite identification of the financial responsibility of patients.
- Better point of service collections.
Practices are able to catch issues related to eligibility early to bridge the gap in care provision.
Automating Prior Authorization Workflows
We are seeing increasingly more automation of prior authority submitting a standard, and the approval to be tracked. Contemporary mechanisms are capable of determining authorization needs according to the payer, procedure, and diagnosis codes and direct the requests through the digital processes.
Robotized authorization applications assist:
- Determine services that will need prior approval.
- Complete payment-related forms with correct information.
- Track authorization and dates out.
- Minimise submissions that are either missed or tardy.
Although the payer rules have not been entirely standardized, automation has minimized manual work and enhanced compliance with authorization.
Financial and Operational Impact
In an event where eligibility approvals and verifications are automated, practices are characterized by minimal preventable denials, reduced accounts receivable cycles, and predictability in cash flow. Employees will be available to spend time on more meaningful procedures like patient interaction and denial prevention instead of spending time on routine administrative duties.
Automation also enhances audit preparedness through the establishment of uniform records of documents and minimising manual workarounds.
The Role of Acuity Health Solutions
Acuity Health Solutions assists the practices to take a strategic advantage of automation, which is combining technology with payer-aligned workflow and qualified management. Risk cannot be eradicated through automation, but a combination of a powerful process design and compliance expertise, it would prove to be a potent tool in protecting the revenue.





